 Cortical thickness and surface area in 3 pre-selected ROIs in each hemisphere were compared between patients with (AH+) and without (AH−) a history of AH and healthy controls (HC). We aimed to determine how auditory cortex thickness and surface area separately relate to AH in schizophrenia spectrum patients. To our knowledge no study has examined the separate relationship between both auditory cortical surface area and thickness, and AH in schizophrenia patients. 32 Sample sizes in studies investigating cortical thickness in relation to AH have been small, and discrepant findings could be due to limited statistical power. Thinner cortex in the “right” HG was reported in 18 first-episode schizophrenia patients with persistent AH compared to 31 first-episode schizophrenia patients who had never experienced AH. A significant association was observed between thinner left STG cortex and increased predisposition towards hallucinations using the Revised Hallucination Scale in patients and relatives, but there was no correlation between Positive and Negative Syndrome Scale (PANSS) hallucination score and cortical thickness. Oertel-Knöchel et al 31 investigated vertex-wise cortical thickness in 31 chronic schizophrenia patients, 29 first-degree relatives, and 37 healthy controls. However, cortical thickness in the HG in the hallucinating group did not differ from controls, and the non-hallucinating patients showed thicker cortex compared with controls. Van Swam et al 30 found reduced cortical thickness bilaterally in the STG and in the left HG among 10 patients with AH compared to 10 non-hallucinating patients. 29Ī limited number of studies have investigated associations between AH and cortical thickness, with mixed results for the auditory cortex. #Primary auditory cortex softwareThe FreeSurfer software allows for automatic reconstruction of the cortical surface from MR images to estimate cortical surface area and cortical thickness. It is therefore of interest to investigate these 2 components independently. 27 Furthermore, thickness and area show different trajectories in the normal aging brain, 28 and may be affected differently by disease processes. Cortical thickness and area are determined by different processes in embryonic cortical development 26 and appear influenced by unrelated genetic mechanisms. Cortical volume is the product of cortical thickness and cortical surface area hence volume alterations may result from altered thickness, area or both. Most previous structural MRI studies have used volumetric ROI 20, 22 or voxel-based morphometry (VBM 17, 19) approaches, reporting data on cortical grey matter volume. 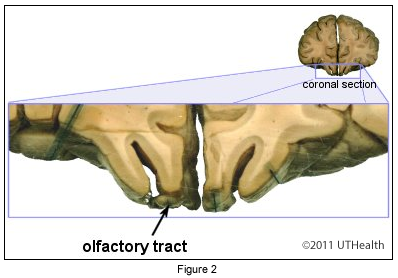
19, 21 However, “larger” grey matter STG volumes in hallucinating compared to non-hallucinating patients have also been reported 22 and still other studies have failed to find associations between severity of AH and grey matter volume in this region. 15, 16 Structural neuroimaging studies have demonstrated associations between greater severity of AH and “smaller” grey matter volumes of HG 17–20 and STG. 6, 12–14 In functional magnetic resonance imaging (MRI) studies, activation in auditory cortex regions was observed in schizophrenia patients while experiencing AH in the scanner. 11 Neuroimaging studies have demonstrated significant associations between AH and structural and functional auditory cortex alterations in schizophrenia patients. 9 The auditory cortex includes the primary auditory cortex (in the Heschl’s gyrus ), 10 and surrounding auditory association cortex in the planum temporale (PT) and the superior temporal gyrus (STG). 5, 8 Evidence suggests that schizophrenia patients show deficits in basic auditory processing that may be consistent with auditory cortex pathology.  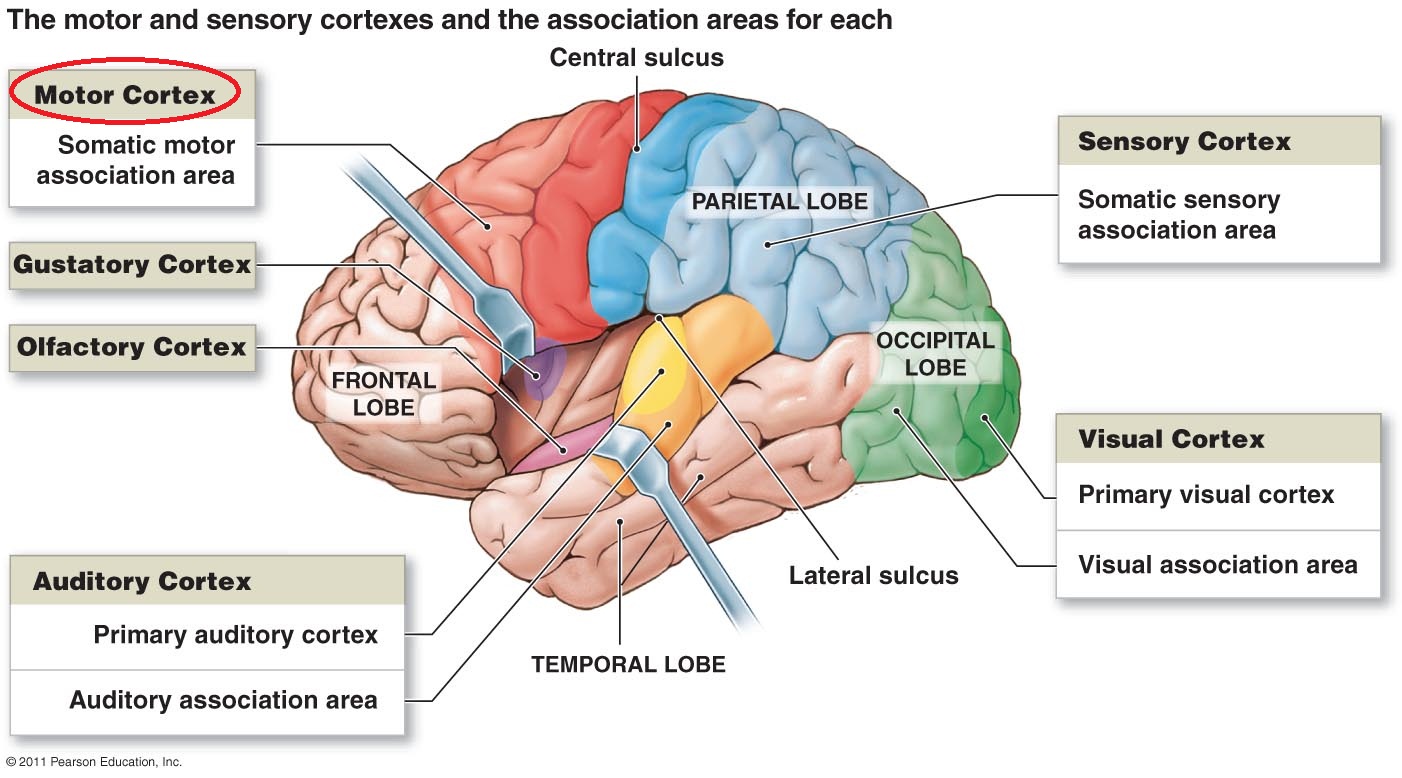
Given the perceptual quality of the AH, the auditory cortex constitute an important region of interest (ROI) for exploring the underlying biological substrate of AH. 4 Despite extensive efforts to elucidate the neural mechanisms underlying AH in schizophrenia patients, 5–7 so far the neurobiological underpinnings remain obscure. In a longitudinal study following 150 psychosis patients for 20 years, 40%–45% of the schizophrenia patients had frequent or persistent hallucinations during this period, 3 and having AH at index hospitalization was associated with a reduced likelihood of recovery over the next 20 years. 1, 2 These false auditory perceptions are often voices with a negative emotional valence, causing the patient great distress. Auditory hallucinations (AH) are the most frequently occurring psychotic symptom in schizophrenia, with a lifetime prevalence of around 70%. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
